 When you want to move, in a sport or daily live activity context, your muscles and central nervous system have to comply with at least the minimal force production requirements to make that happened.
When you want to move, in a sport or daily live activity context, your muscles and central nervous system have to comply with at least the minimal force production requirements to make that happened.
On the one hand, to move your body weight in space your muscles have to produce forces to move your limbs and control your joints. Therefore, it is necessary to have a minimum of muscle mass per muscle group in order to produce and transmit those forces.
On the other hand, your central nervous system (CNS) has to fire enough, which we call neural drive (literally electrical signals) to switch-on the muscles that your brain has decided are necessary to get activated to achieve the desired task.
It is important to understand that in every single movement we produce “active tension” or force, which is the one related to the neural drive and the electrical activity coming from your CNS to your muscles and “passive tension” which is the tension transmitted via your muscles structure, as in the muscle material itself. Therefore, to perform well in life we need stronger muscles as well as an active CNS.
When you have osteoarthritis (OA), neither your CNS nor your muscle belly/tendons are coping well with the minimal requirement of the environment to cope with simple daily life activities such as going up or downstairs.
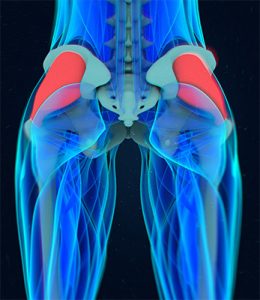
In a study conducted by the University of Kentucky, Lexington, KY, USA, published in the journal Clinical Biomechanics in 2013 was found that people with hip OA tend to activate more their gluteus medium muscles in order to complete sub maximal tasks, as stepping on or off a step compared to the healthy population. The researchers suggest that due to the weakness of the muscle structure, people with OA tend to increase their neural drive to produce the same amount of force than someone with healthy muscles and joint.
In conclusion, someone with OA has to work extra to achieve the same as someone with stronger muscles. This would explain why people express during their sessions a sensation of soreness and tiredness around their hip area after going up or downstairs.
In addition, in the same study, it was found that patients with hip OA push through the ground and into their affected lower limb about 12% more than healthy individuals and up to 19% more than the uninvolved side. Which could explain why going up stair is one of the hardest activities of daily living that these patients have to deal with.
Another study done by Latrobe University, Victoria, Australia, published in the journal of Osteoarthritis and cartilage in 2016 (Hip abductor muscle volume in hip osteoarthritis and matched controls) found that people with OA exhibit a decreased volume of gluteus major, mediums, minimum and tensor facia latae compared to healthy subjects and the unaffected side. Moreover, the levels of fatty infiltration in the gluteus major and medium muscles was higher in the affected side than on the unaffected side. The strength levels of those muscles were significantly reduced as well. These findings show that passive tension production can be affected because people with hip OA simply have less gluteus mass. Similar findings were found in a study conducted by the University of Queensland published in the journal Manual Therapy in 2009 (gramdeli hip). The findings revealed a reduced size of the glute medium and piriformis of the affected side.
The good news is that those muscles can be regained by improving the capacity of producing “passive force” by your muscles structure itself and by activating the gluteus muscles properly so you are not overloading your system when you go up, down stairs or walking.
A tailored resistance training protocol will help you to regained muscle mass to improve your capacity to produce passive tension with them, making the things easy for your CNS and ultimately restoring the balance between muscle tension and neural drive.
Luis Fernandez Astudillo
Senior Physiotherapist at AIM Physiotherapy
Strengthening and Conditioning Coach ASCA
Physiotherapist of the Olympic Team of Chile – Rio 2016